The Challenging Economics of Vaccine Development in the Age of COVID-19, and What Can Be Done About It
Brown University
Brown Center for Biomedical Informatics
QLS Advisors LLC
QLS Advisors LLC
The MITRE Corporation
MIT
QLS Advisors LLC
Santa Fe Institute
he recent destructive outbreak of the novel coronavirus, SARS-CoV-2, that emerged from Wuhan, China, and rapidly spread to Europe and North America, demonstrates beyond doubt that emerging infectious diseases (EIDs) are a clear and present danger to the world and its economy.
Uncontrolled outbreaks of EIDs can devastate populations around the globe, both in terms of lives lost and economic value destroyed. Emerging and re-emerging strains of infectious disease have become more diverse over time, and outbreaks have become more frequent. In 2006, Larry Brilliant stated that 90 percent of the epidemiologists in his confidence agreed that there would be a large pandemic—in which 1 billion people would sicken, 165 million would die, and the global economy would lose $1-3 trillion—within two generations. In 2020, this remarkable statement is playing out with each passing day.
Despite the threat these diseases pose to global health and security, there are few economic incentives for manufacturers to develop preventative vaccines for EIDs. The costs of vaccine development is not dissimilar to research and development (R&D) costs for other disease areas such as oncology, with out-of-pocket costs typically in the hundreds of millions of dollars per project. However, the historical estimated probabilities of success in vaccines is an order of magnitude higher: 3.9 percent in oncology versus 40.6 percent in vaccines (as of 2019 Q4; see https://projectalpha.mit.edu). Therefore, the fact that several biopharmaceutical companies have abandoned the vaccine business underscores the business challenges involved in producing vaccines.
The current COVID-19 outbreak (the disease caused by the coronavirus) should now convince even the most hardened skeptic that vaccine development can no longer be crisis-driven. While non-profit organizations such as the Coalition for Epidemic Preparedness Innovations (CEPI), the World Health Organization (WHO), the Gates Foundation, and the Wellcome Trust have contributed significant resources to vaccine development, philanthropy alone is not sufficient. The public health aspects of pandemics can only be addressed effectively through government action, including a viable, sustainable model that will align the financial incentives of stakeholders to encourage the necessary investment in vaccine development.
Megafund Rationale
Several mechanisms have been proposed to create incentives for industry to develop EID vaccines and other medical countermeasures. They include the direct government acquisition of stockpiles of vaccines, priority review vouchers for their R&D, and the establishment of advance market commitments for newly developed vaccines. Beyond the push of significant R&D support, these mechanisms provide some measure of a pull. However, to date, none of these strategies have been effective.
If traditional market forces are unable to meet the needs of EID vaccine development, might non-traditional methods take their place? A “megafund” strategy—raising a multi-billion-dollar fund using techniques like portfolio theory and securitization—can attract large-scale financial resources to fund the development of a portfolio of drug development programs by using securitization to reduce investment risk in these assets. We explore this possibility in a recent paper by simulating the financial performance of a hypothetical megafund portfolio of 141 preclinical EID vaccine development programs proposed by CEPI across nine different EIDs for which there are currently no approved prophylactic vaccines. We provide a brief summary of our findings below.
The basic structure of a megafund involves creating a financial entity that issues debt and equity (e.g., bonds and stock) to investors. This entity will then use the raised capital to invest in a portfolio of underlying assets, in this case, vaccine candidate programs targeting EIDs. In this hypothetical megafund, these programs will serve as collateral for the debt—the same way that a car serves as collateral for an auto loan—and their future cash flows will pay the interest and principal of the issued bonds. Once the debt has been repaid, whatever is left goes to the megafund’s equity holders.
The securitization of vaccine development enables investors to invest in many vaccine projects at once, thus increasing the likelihood of at least one success. This in turn reduces their risk of financial loss. The megafund’s large and diverse asset portfolio permits the issuance of debt, which is critical because bond markets contain much larger amounts of investment capital than venture capital, or private- and public-equity markets. This larger capacity allows the megafund to raise enough funding to purchase a sufficiently large number of assets to reach its critical threshold of diversification.
We chose the target diseases from the Priority Pathogen list prepared by CEPI and its portfolio assets from pipeline research for each disease. We made several assumptions about the cost of vaccine development (a net present value of $250 million per project, a total of $35.25 billion for the portfolio), the probability of success of each project (32 percent through phase 2 clinical trials, according to CEPI estimates), and a subtle but important factor, the pairwise correlations of success among the projects, which are essential to simulate the level of diversification in the portfolio.
We also made several assumptions to project future revenues. The prophylactic regimen would consist of a single dose of vaccine. The probability of disease outbreak was based on historical outbreaks per disease, while regimen demand was projected using historical outbreak size, potential for pandemic spread, and an assessment of relative clinical severity. The price per regimen was based on whether the disease in question typically affected high-, medium-, or low-income countries, using CDC, GAVI, and Pan American Health Organization (PAHO) vaccine pricing data. Herein lies the problem: although the cost of vaccine development is comparable to the cost of drugs for other diseases, the estimated price per dose of an EID vaccine ranges from $1.97 for Lassa fever in a low-income country to $46.12 for MERS in a high-income country. Compare these potential revenues of a cancer drug—in 2012, 11 of the 12 drugs approved by the FDA for treating cancer were priced at over $100,000 per year.
The simulated investment performance of an EID vaccine portfolio as a function of the commercial potential of each individual vaccine project is illustrated in Figure 1. The investment returns of these vaccines are consistently very poor, orders of magnitude lower than what would be required to make them commercially viable. The simulation parameters that are closest to industry estimates result in a net present value of only $7.6 million per successful EID vaccine—two to three orders of magnitude less than that of a typical cancer drug—and the vaccine portfolio’s overall expected return is −61.1 percent. Simply breaking even would require selling vaccines at approximately 100 times the price assumed in our simulations. We provide a similar financial simulation for the impact of combining the EID vaccines portfolio with an otherwise profitable pharmaceutical company. The vaccines business imposes an unsustainable drag on performance under historical cost and revenue assumptions.
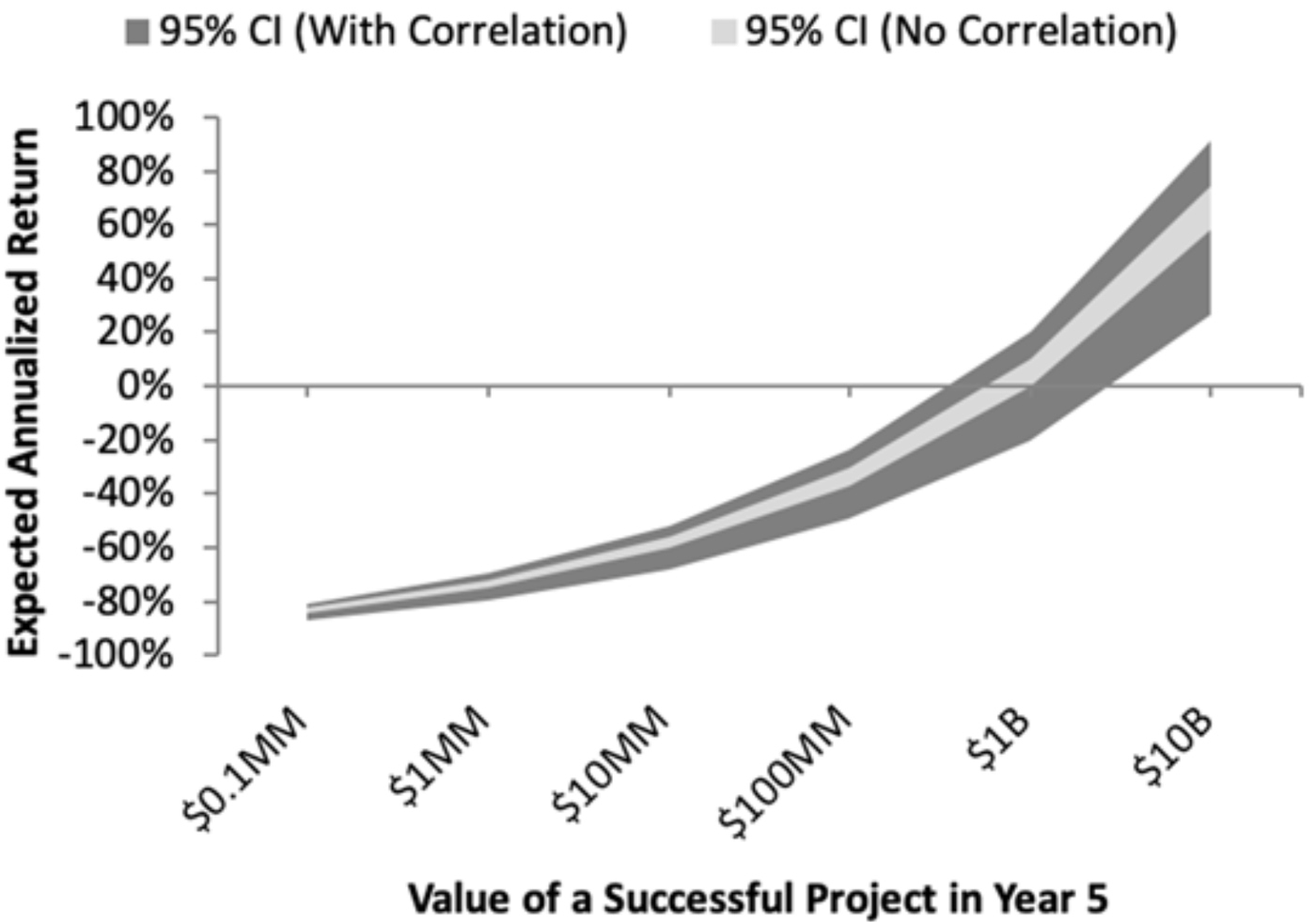
Our results are consistent with the biopharma industry’s trend towards fewer companies willing to engage in vaccine development. Given current cost and revenue estimates, a private-sector EID vaccine portfolio seems infeasible, underscoring the need for some form of public-sector intervention. Unless these challenges are addressed, the global population will remain vulnerable to substantial human and economic losses when epidemics and pandemics arise.
Discussion
A weak and uncertain market demand led to a lack of interest in developing vaccines against EIDs prior to the current COVID-19 crisis. This indifference has left the global community increasingly vulnerable to repeated outbreaks of these viruses. The challenges of EID vaccine development are troubling issues for vaccines more generally, since there are only four remaining major pharmaceutical companies engaged in vaccine development.
Vaccines sell for a fraction of their economic value, in some cases for only a few dollars per dose despite often offering a lifetime of protection from a given disease. The low price may benefit individuals and regions with lower incomes, but in the long run, it has had the opposite effect, causing them to be medically underserved due to a lack of vaccine investment. Pharmaceutical companies and investors now direct their resources to projects in which the estimated return on investment is more predictable and lucrative.
However, the societal value of vaccines is enormous, and the investment required to reduce the global risk from EIDs is actually within reach. Securing these resources will require governments to strengthen their commitments to supporting EID vaccine markets. Government engagement is integral for long-term pipeline sustainability. Public policy can catalyze private sector investments through a range of strategies, including guaranteed commitments. The US government’s Medical Countermeasures (MCM) program has demonstrated a capability to create incentives for the development of vaccines that would otherwise not be developed by guaranteeing sufficient market demand ahead of time. The government provides market commitments on the order of $100-200 million per year for successful vaccine development programs for anthrax, smallpox, and various strains of pre-pandemic influenza.
While political challenges exist in sustaining these funding commitments, they are clearly one part of the public-private solution to EID vaccine development. Fifteen years of guaranteed revenue via purchase commitments, similar to the US government’s purchase of smallpox and anthrax vaccines, would catalyze these development efforts. For example, an annual purchase commitment of $150 million per successful vaccine candidate would represent a net present value of $1.14 billion, exceeding our calculated breakeven value of $772 million.
Another key to the problem of EID vaccine funding is in the pricing of the risk of infection by EIDs. Although the prevention of epidemics and pandemics saves countless lives and billions of dollars of economic value, the revenue realized by vaccine manufacturers is far below the amount to sustain the necessary research and development. With this in mind, a subscription model applied to vaccine development seems promising.
Under the current model, vaccines are purchased a la carte after outbreaks begin. However, if nations, health organizations, and other stakeholders were to pay in advance to develop and stockpile vaccines, the amount of capital needed to fund these programs would be easier to raise and would keep the price per regimen lower. These subscriptions can be viewed as a form of insurance that would maintain epidemic response capabilities and provide protection from EID outbreaks, much like a society-wide immune system. Vaccine developers under this model would sell subscriptions to governments, building upon existing infrastructure, such as the US government’s biodefense and pandemic preparedness programs.
Consider a subscription model under which the largest governments around the world agreed to purchase subscriptions to EID vaccines on behalf of their constituents. Suppose that the governments of the G7 countries agreed to pay a fixed subscription fee per capita over a fixed amortization period to cover this cost. How much would this subscription fee be? For an amortization period of five years, and an estimated total G7 population of 770 million and a cost of capital of 10 percent, we estimate the per capita annual payment to cover the total cost of $35.25 billion to be only $12.08 per person per year. As a percentage of the annual per capita healthcare expenditure of each G7 country, the cost is trivial for all countries, ranging from a high of 0.59 percent for Italy to a low of 0.15 percent for the US.
As devastating a tragedy as COVID-19 has been, it may serve as a much-needed catalyst to convince governments to act in unison to implement a sustainable solution to EIDs once and for all, preventing even greater devastation in the future. Let us honor those who lost their lives in the current pandemic by ensuring that their descendants will avoid a similar fate.
Please address all correspondence to Andrew W. Lo, alo-admin@mit.edu.

